Perimenopause and the Pelvic Floor
Perimenopause and menopause are phases of life that are often characterized by wildly variable symptoms from insomnia, to changes in body composition, to hot flashes, and everything in between. Everyone has a different experience with this phase of life and it can be overwhelming to figure out a course of action to support your own experience.
In this blog, I would like to touch on the most common diagnoses and symptoms I come across as a pelvic floor physical therapist and give you tangible action items that will empower you to take control of your perimenopause experience and live your best life with confidence!
Before we get there, though, let’s start with some of the basics:
What is Perimenopause and Menopause?
Menopause is a single period of time in which menses has not occurred for a full 12 months. Anything after that point in time is considered post-menopause and anything before the onset of menopausal symptoms is considered pre-menopause. So that brings me to the obvious next question…what is perimenopause?
Perimenopause is the transitional period leading up to menopause. It commonly starts between the ages of 45-55 and can last up to 15 years, though the age of onset and duration is highly variable between people. During perimenopause, Estrogen and Progesterone production steadily decline. The decline in the production of these hormones ultimately leads to the symptoms that many experience. Some of the most common symptoms include:
- Hot flashes
- Night sweats
- Insomnia
- Changes in sexual desire
- Bleeding with intercourse
- Vaginal dryness
- Urinary incontinence
- Changes in body composition
- Anxiety
- Depression

How do changes in Estrogen affect the pelvic floor?
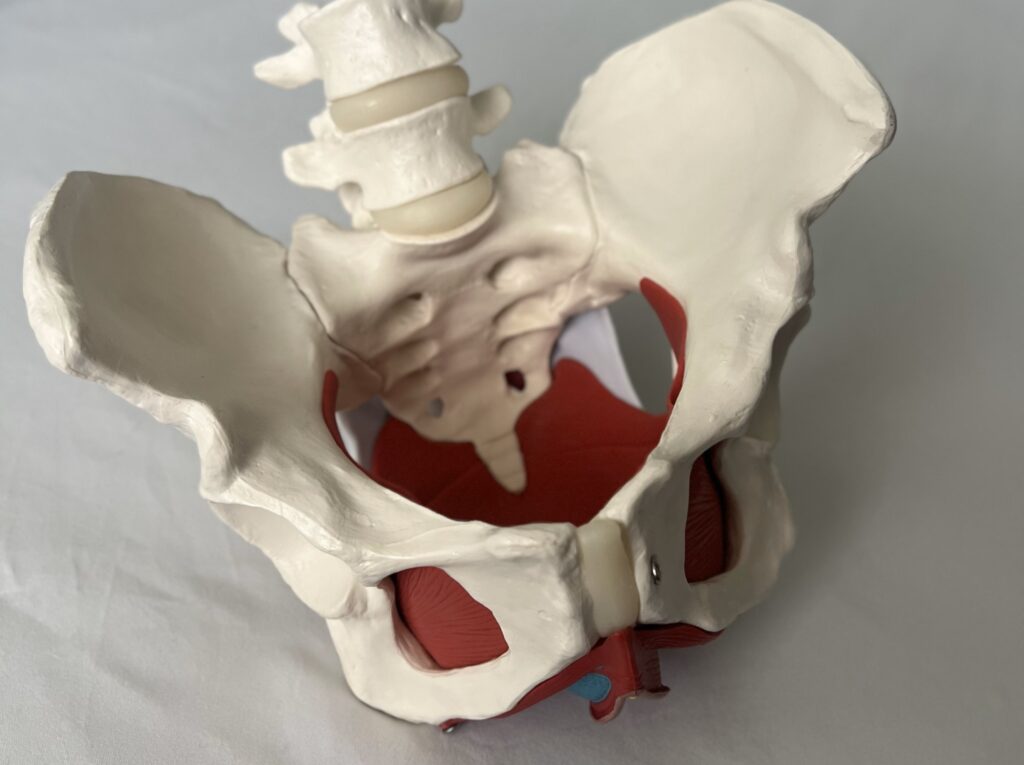
The pelvic floor musculature, vulva, and surrounding tissues contain a very high number of Estrogen receptors, which ultimately makes them highly sensitive to changes in estrogen levels. During perimenopause, as estrogen steadily declines, the pelvic floor musculature becomes less compliant, thinner, and weaker. In addition, the vagina’s natural lubrication decreases, making the vulva and vaginal tissues drier, prone to infection, and prone to irritation from intercourse and clothing.
Common symptoms of Perimenopause
By far the 3 most common symptoms I treat in this population are 1) urinary incontinence, 2) pelvic organ prolapse, and 3) pelvic pain.
1. Urinary Incontinence
As mentioned previously, as estrogen declines, the pelvic floor becomes weaker and less compliant. This leads to difficulty in recruiting the pelvic floor to help manage increases in pressure in the abdomen and pelvis.
For example, when you cough or sneeze, the sudden forceful contraction of your abdominal muscles leads to a sharp increase in pressure in the abdomen. Normally, the pelvic floor would contract to help contain this pressure. However, when it is weakened by a decline in estrogen as in perimenopause, it is unable to contract as strongly, which leads to an inability to contain the sharp pressure increase and ultimately leads to urinary leaking.
While urinary incontinence is an extremely common symptom of perimenopause, it certainly is not normal and shouldn’t be tolerated as “just part of aging”. So, here are a few tips I give to treat urinary incontinence:
1. Avoid bladder irritants – Common bladder irritants include caffeine, alcohol, carbonated beverages, citrus, sugar/artificial sweeteners, and chocolate. While it may not be necessary to entirely eliminate these, it is helpful to understand that consuming these items can lead to irritation of the bladder lining and worsening or urinary incontinence symptoms. Moderation is key!
2. Stay hydrated – It is recommended to drink 0.5 – 1 oz of water per pound of body weight every day. Be sure to consider factors like sweating. That is, in the hot summer months when you are sweating more, it is best to aim for closer to 1 oz per pound of body weight.
3. Strengthen the pelvic floor – Even though declining estrogen levels results in a weaker pelvic floor, that does not mean it cannot be strengthened! While you may not have had to specifically focus on strengthening your pelvic floor in your child-bearing years, there comes a time when it should become a focus in your regular routine. Strengthening your pelvic floor does not necessarily mean doing repeated, isolated Kegels, but also includes regular strengthening of your inner thighs, glutes, and abdominals, which are all muscle groups that support the pelvic floor.

4. Improve pelvic floor coordination – I’ll admit, this one is a lot more elusive and challenging to incorporate on your own without specialized guidance from the pelvic floor specialist. However, your focus should be to consciously perform a Kegel a split second before you cough, sneeze, laugh, lift, or jump. This will improve your ability to manage the increase in intraabdominal pressure and prevent leaking.
2. Pelvic Organ Prolapse
Pelvic Organ Prolapse (POP) is when weakening of the vaginal wall, in this case from the decline of estrogen during perimenopause, results in one or more pelvic organs bulging into the vaginal canal. This can lead to feelings of pelvic pressure or heaviness and occasionally difficulty emptying your bowels or bladder. These symptoms are often best in the morning or after a period of laying down. They often get worse as the day goes on or after long periods of upright activity.
Here are a few tips I give to help manage POP symptoms:
1. Pressure management – With POP, you want to limit tasks that introduce downward strain on your pelvic floor. These include repetitive jumping, holding your breath when exerting, and less-controllable things like coughing, sneezing, and laughing. In addition to the strategies of strengthening the pelvic floor and improving pelvic floor coordination as mentioned above, you can also focus on maintaining a consistent breathing pattern while exerting, rather than holding your breath. Examples include avoiding holding your breath while strength training (especially while training abdominals) and avoiding holding your breath while pushing to pass a bowel movement.
2. Keep stool consistency regular – When your stool is firm and harder to pass, you become more prone to holding your breath and bearing down to empty your bowels. This introduces a ton of downward pressure on the pelvic floor, which can in turn worsen POP symptoms. It is advised to stay hydrated and to avoid anything in your diet that knowingly leads to constipation.
3. Use pessaries as needed – A pessary is like a “sports bra” for your pelvic organs. It is a small object that you insert intravaginally to help support the vaginal walls and pelvic organs. Pessaries come in many different shapes and sizes depending on the nature and severity of the POP, so it is recommended you get one custom fitted by a professional at your gynecologist’s office.
4. Gravity training – It can be helpful to counteract long periods of upright activity with bouts of laying down with your pelvis elevated and your legs on a wall as shown. With your pelvis elevated, you can use gravity’s help to offload the pelvic floor.

2. Pelvic Pain
Pelvic pain is a massive term that can mean so many different things. However, the most common types of pelvic pain I see in the perimenopause population have to do with vaginal dryness. As mentioned previously, the decline in estrogen makes vulvar and vaginal tissues drier and more fragile, which can lead to itchiness, irritation, pain, and bleeding. This can often go hand in hand with painful intercourse and/or bleeding during and after intercourse.
Here are a few tips I give to manage pelvic pain as it relates to vaginal dryness:
1. Use vaginal estrogen – Vaginal estrogen, or Estradiol, often comes in the form of a topical cream that can be applied in the vagina and around the vulvar tissues. It is prescribed by a physician, so ask your doctor if this option is right for you!
2. Use a vaginal moisturizer – Vaginal moisturizers are often over-the-counter topical creams, gels, and/or ointment that help moisturize the vulvar tissues and combat any dryness or itchiness that occurs as a result of declining estrogen. Some brands I recommend are Feel Amazing, Good Clean Love, and Medicine Mama’s VMagic.
3. Use lubrication during intercourse – Lubrication during intercourse can be extremely helpful in reducing friction and skin irritation, which not only cuts down on discomfort, but it will also reduce any bleeding that might normally occur. Brands I recommend include Good Clean Love, Maude, and Slippery Stuff.
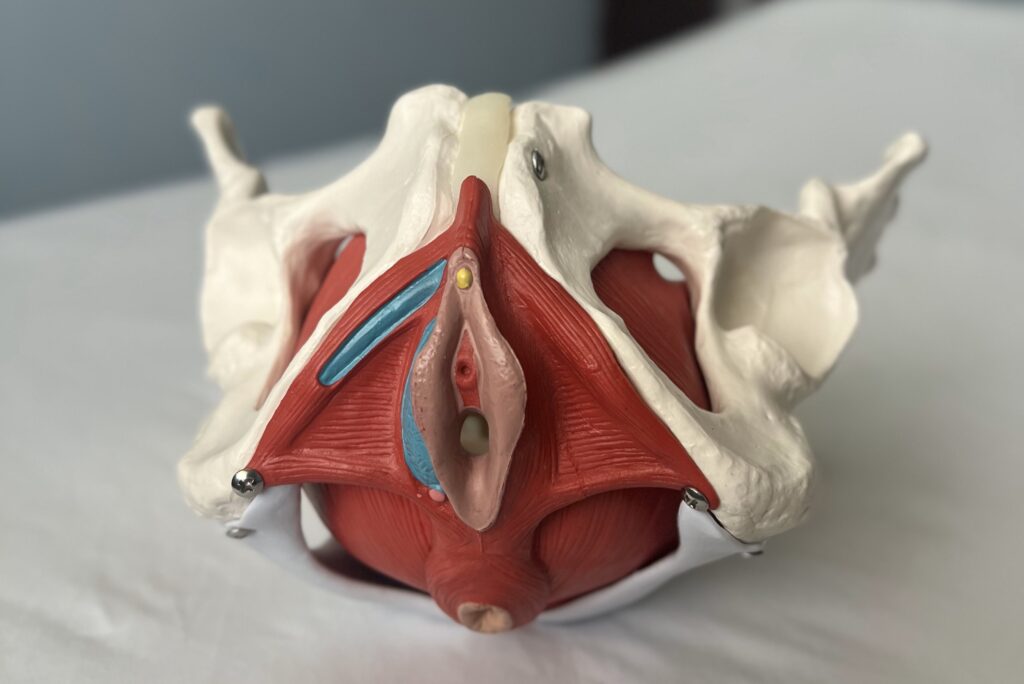
While urinary incontinence, pelvic organ prolapse, and pelvic pain are the most common symptoms I come across in the perimenopausal population, there are many more symptoms and presentations that are appropriate for pelvic floor physical therapy. So, if you would like individualized guidance that takes into account your unique history, goals, and needs, click the link below to talk to one of our Pelvic Physical Therapy specialists!
Contact Us Today
Not sure where to start?
Schedule your free 15-minute consultation.
Returning client or ready to get started with therapy today? Call us to schedule your appointment.
